Abstract
Background: The AHL2011 study demonstrated that a PET-driven strategy allows to deescalate treatment to 4 x ABVD in PET negative patients after 2 cycles of escalated BEACOPP (BEACOPPesc) without loss of tumor control in patients with advanced Hodgkin lymphoma (HL) compared to a non PET-monitored treatment delivering 6 x BEACOPPesc (Casasnovas RO et al, Lancet Oncol 2019). The interim PET results after 2 (PET2) and 4 (PET4) cycles of chemotherapy were found to influence patients PFS and OS independently of IPS. To further refine the patients outcome prediction we evaluate the prognostic value of baseline Total Metabolic Tumor Volume (TMTV) and tumor dissemination (SDmax) in Ann Arbor stage III-IV patients included in the AHL2011 trial.
Patients and methods: 634 patients enrolled in the AHL2011 trial with stage Ann Arbor III or IV were included in the study. According to the AHL2011 trial, patients were randomized in a standard arm (6 x BEACOPPesc) or a PET-driven arm (2 x BEACOPPesc and 4 x ABVD in negative PET2 patients or 4 x BEACOPPesc in positive PET2 patients). For each patient, a semi automatic tumor segmentation was retrospectively performed in baseline PET to calculate TMTV using the 41% of SUVmax threshold and compute the maximum distance between the delineated lesions normalized by body surface area (SDmax). Optimal thresholds for TMTV and SDmax were calculated using X-Tile and ROC curve approaches in a randomly assigned training (n=317) and validation sets (n=317). The per protocol PET2 and PET4 responses were analyzed using the modified Deauville criteria (positive if residual uptake >140% background liver). Multivariate analysis included treatment arm, TMTV, SDmax, international prognosis score (IPS), PET2, and PET4 as covariates. The median follow-up was 5.6y.
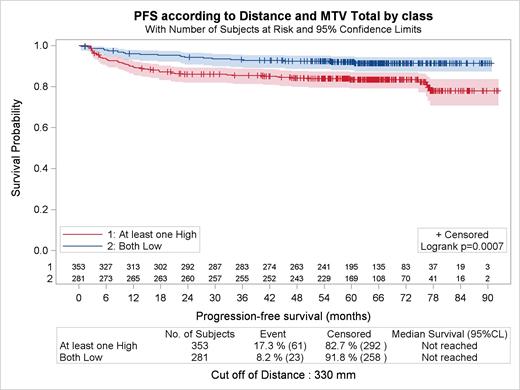
Results : Median TMTV and SDmax were 215 ml and 0.221 m-1 in the whole population and similar in both randomized arms and in the training and validation sets. Optimal cutoffs were 220ml for TMTV (312 patients [49%] had High TMTV) and 0.330 m-1 for SDmax (149 patients [24%] had High SDmax) and similar in the training and validation sets. 5-year PFS for patients with TMTV>220ml was 84.1% vs 90.2% in low TMTV patients (p=0.02) in the whole population (in the training set: 83% vs 89%, p=0.088 ; in the validation set : 86% vs 92% p=0.11). 5-year PFS was significantly lower in patients with SDmax>0.333 m-1 (78.8% vs 89.7%; HR=2.15 [95%CI: 1.38-3.35], p=0.0005) in the whole population (in the training set: 77% vs 89%; p=0.0037); in the validation set: 81% vs 91; p=0.046). The combination of TMTV and SDmax allows to identify two subgroups of patients, those having both low TMTV and low SDmax (n= 281; 44%) and those having high TMTV and/or SDmax (5-year PFS: 92% vs 83.4%; HR=2.24 [95%CI: 1.39-3.62], p=0.0007) (figure 1). In multivariate analysis, high TMTV (p=0.034), high SDmax (p=0.0002), PET2 (p=0.02) and PET4 (p<0.001) positivity retained independent prognostic value for predicting PFS.
Conclusion: Tumor burden (TMTV) and dissemination (SDmax) assessed on baseline 18FDG PET allow to predict, independently of early reponse to treatment, the outcome of patients with advanced HL. These two parameters overcome the prognosis value of IPS and could be included into new prognostic scores to tailor personalized therapy in advanced Hodgkin Lymphoma.
Figure 1 : PFS according to TMTV and SDmax in stage III-IV HL patients enrolled in the AHL2011 study
Brice: Takeda: Consultancy, Honoraria, Research Funding; BMS: Honoraria; MSD: Honoraria. Ghesquieres: Janssen: Honoraria; Mundipharma: Consultancy, Honoraria; Roche: Consultancy; Celgene: Consultancy, Honoraria; Gilead Science: Consultancy, Honoraria. Stamatoullas-Bastard: Takeda: Consultancy. André: AbbVie: Other: Travel/accomodation/expenses; Roche: Other: Travel/accomodation/expenses, Research Funding; Johnson & Johnson: Research Funding; Incyte: Consultancy; Gilead: Consultancy, Other: Travel/Accommodations/Expenses; Karyopharm: Consultancy; Bristol-Myers-Squibb: Consultancy, Other: Travel/Accommodations/Expenses; Celgene: Other: Travel/accomodation/expenses; Takeda: Consultancy, Research Funding. Rossi: ROCHE: Honoraria, Research Funding; Takeda: Honoraria; JANSSEN: Honoraria; ABBVIE: Honoraria. Casasnovas: Roche: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; Takeda: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; Gilead Kite: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; MSD: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees; BMS: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees; Amgen: Consultancy, Honoraria; Janssen: Consultancy, Honoraria; Abbvie: Consultancy, Honoraria.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal